As anyone who experiences or has loved ones who share fibromyalgia knows, it is excruciating. People living with fibromyalgia sometimes describe the sensation as achy or as if they’ve strained their muscles.
Some would even describe it as a burning or stabbing sensation. Regardless of the type of sensation, the part of the body most affected is the muscular system. Our muscles are what enable us to move our body parts.
They are essential to our everyday functions and capabilities to do almost anything. Therefore, people who suffer from this uncomfortable and painful condition are significantly inhibited in their abilities to do certain things.
Many patients describe the formation of muscular knots around their body, called fibro knots. They are mostly centered around their shoulders, neck, and back.
However, it is arguable whether these knots result from fibromyalgia, or myofascial pain syndrome (MPS), as they are known as myofascial trigger points and are generally not widespread pain.
So are these nodes caused by or do they go hand in hand with fibromyalgia? Or are they two separate disorders entities fighting in the same body?
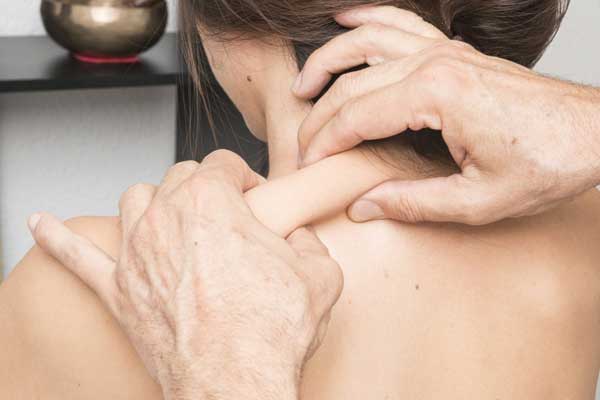
What are Muscle Knots?
Muscle knots are a type of spasm in which a small portion of a muscle becomes tense and painful. Such knots typically occur when the power is stressed due to repetitive motions or when it’s held in an awkward position for too long.
While researchers are still trying to figure out exactly why muscle knots cause pain, some think it could be due to restricted blood flow or triggered nerves.
Muscle knots can be painful and linger for days, making it difficult to do activities you enjoy. Stretching, massage and other therapies are effective treatments for muscle knots.
Differences in Fibromyalgia and MPS
While the symptoms of fibromyalgia are well-known in the medical world, what causes them and what is happening in the body are not as easily found.
According to experts, fibromyalgia is a chronic disorder that causes constant fatigue, pain, and discomfort in the muscles in tender points of the person living with it.
The patient must suffer pain in at least 11 of the 18 tender points to be diagnosed with fibromyalgia. Some people believe fibromyalgia is not a real disorder but a product of the mind of the person suffering from these symptoms.
On the other hand, MPS is a result of overuse of or injuries to muscles, resulting in the formation of tight muscle fibers and tissues (nodes or knots).
These knots and points of pain are known as trigger points. When touched or irritated, the pain can spread throughout the muscle into different body parts.
This pain is not generalized throughout the body but is usually centered in one or a few specific body muscles.
Tender Points Versus Trigger Points
As stated above, one of the differences between fibromyalgia and myofascial pain syndrome is the presence of tender points and trigger points.
In fibromyalgia patients, there are 18 tender points spread all over the body. These are particular spots that are extremely sensitive and very painful when pressure is applied. Out of the 18 tender points, at least 11 must be painful to diagnose fibromyalgia.
Trigger points are a bit different. While still painful, the pain is often redirected to another part of the body when pressure is applied, even if the point itself is not tender or sore.
A trigger point can also be located anywhere on the body. That is to say that it can be found in any skeletal muscle. Also, while several tender points are present in the body, it is possible only to have one trigger point.
Similarities in Fibromyalgia and MPS
Because of the similar symptoms in the two and the fact that, in many cases, the two disorders overlap, they can often be confused for one another or thought of as the same disorder. This can result in the diagnosis and treatment of just one of these conditions.
Unfortunately, the two treatments are very different, which means that if they are confused, the patient may not receive the correct treatment and may have to continue living in pain until the proper diagnosis has occurred.
Both conditions cause:
- Muscle pain
- Sleep disturbances
- Headaches
- Memory problems
As one can see, they share many symptoms, making it easy to mistake one for the other. However, they are not the same and should be treated as two separate conditions to rid the sufferer of all symptoms.
One other thing that some people might argue that these illnesses have in common is knots or nodes that form in the muscles. Many sufferers of both conditions refer to knots inside the muscles that cause pain and restrict the movement and use of muscles.
While in the case of MPS, these knots are trigger points, some people with fibromyalgia refer to them as fibro knots.
It is unclear, however, if these knots result from someone who suffers both conditions simultaneously or not. If this is the case, the knots are likely to trigger points. But some people firmly believe these are fibro knots and are directly related to fibromyalgia.
The truth is, it is hard to tell if they are two separate entities or one or the other. This is because fibromyalgia and myofascial pain syndrome often occur together, making differentiation difficult.

Fibro Knots: Fact or Myth?
It is debatable whether or not fibro knots exist. As was previously stated, fibromyalgia and myofascial pain syndrome can co-occur, making it very hard to differentiate between the symptoms of each condition.
Some people very much believe fibromyalgia can cause sore, tight nodes or knots deep inside the affected muscles, AKA fibro knots. However, others would argue that this is a myofascial trigger point.
Experts are not sure why it is common to suffer from both illnesses simultaneously, as they cannot find an actual common factor. However, it seems to be a recurring pattern, therefore creating a mixture of symptoms that are hard to distinguish between.
In such cases, there is quite a bit of controversy as people have made up their minds and are sure of what they are experiencing, not to be told any differently by anyone—especially someone who is not experiencing their pain.
Therefore, the subject of fibro knots is uncertain. Fibro knots are described as deep knots or nodes in the muscle tissue that restrict movement and cause pain when touched.
This description also fits myofascial trigger points, clouding the air a bit when differentiating between the two. Until experts discover scientific proof one way or another, it will remain a medical mystery.
How to Treat Muscle Knots
Muscle knots can cause significant pain and discomfort, but they can be managed at home with patience and persistence. Stretching regularly and being aware of common trigger points can help prevent muscle knots from forming.
When dealing with an existing knot, alternating between cold and hot compresses and applying firm pressure can help. If the pain persists, visiting a professional massage therapist may be necessary to get complete relief.






